This post is also available in Dutch.
Turning specific brain areas ON and OFF for the treatment of depression, sounds as mechanic as handling a thermostat when turning on the heat. Researchers have some hopeful news for patients with depression: For many, their mood can be controlled by a brain electrode.
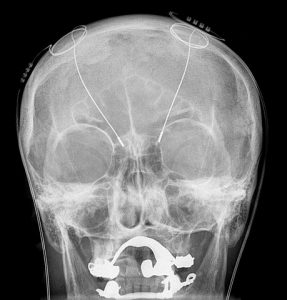
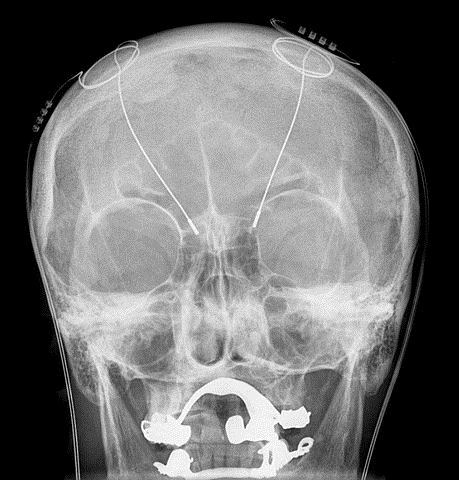
By Hellerhoff ([CC BY-SA 3.0]), via Wikimedia Commons.
A radiogram of a patient with deep brain stimulation electrodes inside the brain
In 2015, Emory Medicine magazine described a women who suffered from the depression after pregnancy “The darkest day of Marjorie Stowe’s depression came when her long-time psychiatrist told her she obviously was choosing to resist the healing effects of one medication after another and psychotherapy. Her gynecologist told Stowe about an Emory neurologist who was doing a special type of brain surgery, ‘You have a physical illness of the brain, this might be your best hope,'” (Citation from emorymedicinemagazine).
Deep brain stimulation as treatment for depression
Depressive patients like Marjorie Stowe have an overactive part of the brain, called area 25, which was discovered by a neurologist named Helen Mayberg from Emory University in Atlanta. This area plays a role in the control of mood and is connected to parts of the brain regulating processes known to be dysregulated in depression (e.g. sleep, motivation). The delivery of an electrical current to area 25 could block its overactivity and therefore relieve depressive symptoms.
How does deep brain stimulation work?
This electrical current is delivered to area 25 by means of deep brain stimulation, or DBS. With DBS, surgeons place tiny electrodes in specific brain areas that are connected to a pacemaker-like device implanted in the chest. The pacemaker can be programmed and controlled from outside the body by a handheld device.
Scientific evidence showed 66% success rate of DBS in depression
Depression, a mental disorder characterized by low mood or loss of interest or pleasure in daily activities, ranks amongst the top causes of global burden of disease. While most patients are well treated with medication or psychotherapy, 20% of patients remain treatment resistant. It is for those patients who remain resistant that DBS could be a last resort.
A study published in the scientific journal Neuron showed that 66% achieved long-lasting remission at the end of 6 months after DBS. Given the extreme treatment refractoriness of this patient population, this is a promising result.
66% is not 100% percent: there are limitations
Depression is a very complex disease, with different comorbidities and causes. It is unlikely a result of a dysfunction of one single part of the brain. This variability makes it difficult to find a general form of stimulation that works for everyone. It could even be the case that there is one optimal tuning frequency for a given person.
More time and research is needed to unravel the mysteries of thermostat-like brain electrode that turns up the mood and minds of treatment-resistant depressive patients.
More information:
The scientific journal Nature on the opportunities of DBS in the clinical and research context
The Scientific American about the failures of DBS
Youtube film on how deep brain stimulation works
Ted talk on DBS in Parkinson’s and depression from one of the pioneer neurosurgeons at the Univerity of Tornoto Andres Lozano
Written by Mahur.